For decades, scientists have suspected that contracting the virus that causes mononucleosis, the Epstein-Barr virus, greatly increases the risk of developing multiple sclerosis—an autoimmune disease affecting the central nervous system. A series of studies published together in the prestigious journal Cell reveals the connection between the virus and multiple sclerosis. The studies explain not only the mechanism, but also why the disease emerges in only a small subset of those infected with EBV.
Advertisement
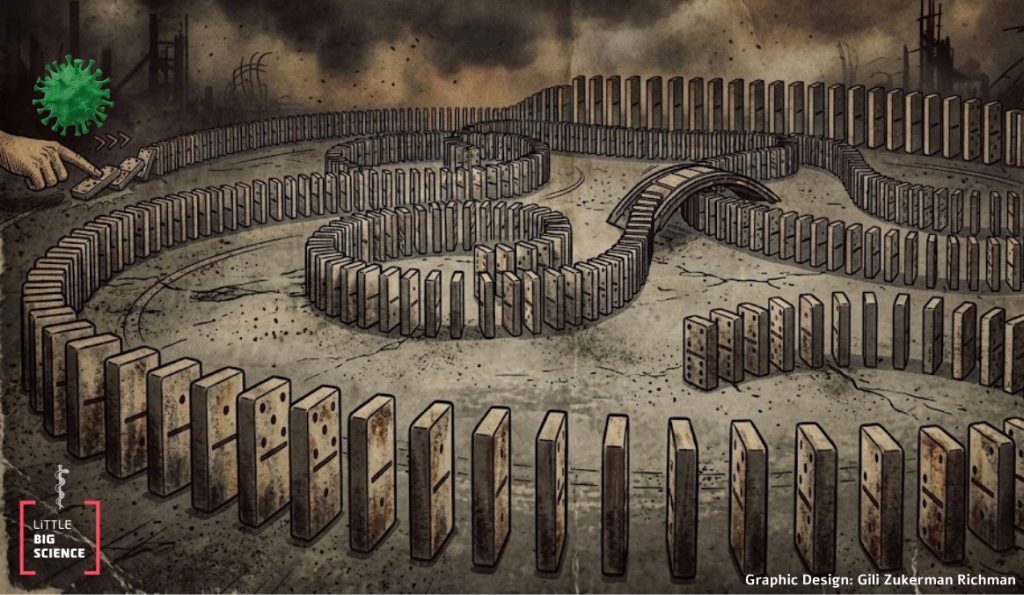
Multiple sclerosis (MS) is an autoimmune disease in which the immune system attacks myelin, the insulating layer that protects nerve fibers. Without proper insulation, the transmission of signals between neurons is disrupted, leading to impairment of motor function, cognitive abilities, and vision [1]. For years it has been known that almost 100% of people with MS were previously infected with the Epstein-Barr virus (EBV). This herpesvirus persists in its latent form in most of the population and, in some individuals, causes the illness colloquially known as “mono“" or “the kissing disease”.
Four years ago, a study following 10 million U.S. military service members for 20 years was published. The researchers tested the presence of two hundred different viruses in blood samples collected at various times, and found that 97% of the service members who later developed MS had antibodies against EBV [2,3]. While EBV infection is very common and about 90% of adults have been infected with it, multiple sclerosis is quite rare, appearing in only about 0.03% of the population. Thus, even if there is a direct link between the virus and MS, the explanation for MS development would not be complete without understanding what distinguishes the people who do develop it.
Three new studies published back-to-back attempted to clarify the mechanism connecting EBV infection with MS and to explain why such a common virus leads to a severe disease in only a small subset of people.
The first study focused on B cells, immune cells that specialize in producing antibodies against specific foreign invaders [4] and are also the type of cell that EBV infects. A study published a few years ago first demonstrated a biological link between these cells and MS. The study found that infected B cells produce a viral protein that resembles a myelin protein. The similarity causes the body to mistakenly make antibodies that mark myelin-producing cells for destruction [5,6]. Under normal circumstances such cells do not survive, because the immune system detects the error and eliminates the rogue cells before they cause harm. The current study is the first to reveal a mechanism that prevents this elimination: EBV causes the infected B cells to express a protein that makes them resistant, turning them into a kind of “Trojan horse” within the immune system. This allows them to proliferate and survive long-term. When brain tissue is inflamed it becomes more permeable, enabling the Trojan B cells to infiltrate and contribute to a concerted immune attack on myelin in the brain [7].
The second study examined T helper cells (CD4+), which trigger destructive mechanisms once they recognize an invader [8]. Each T cell responds to one specific foreign protein and it recognizes it by binding to a receptor on a cell presenting that protein. If the T cell detects its unique foreign marker, it sounds the alarm and recruits the immune system to attack. In people with MS and other autoimmune diseases, T cells mistakenly recognize the body’s own proteins as foreign and attack the cells that express them.
In individuals infected with EBV, the T cells recognize the viral protein and activate the immune response against it. Unfortunately, the receptor that these T cells recognize is very similar to a receptor found on brain cells involved in myelin production. Consequently, the T cells respond efficiently to both the viral and the neural receptors. In a mouse model of MS the researchers showed that this dual action accelerates disease development [9].
These findings, then, beg the question: Why does only a tiny fraction of infected people (about 0.3–0.5%) go on to develop MS? In the third study the researchers conducted a wide genomic analysis that examined the relationship between a genetic variant in the HLA system, which known to increase MS risk, and disease development. HLA proteins act as markers that allow the immune system to distinguish self from non-self, essentially an ID for the cell. In a certain group of people carrying a unique HLA variant, the immune system tends to be more sensitive, more easily convinced by the erroneous information, and therefore to identify the myelin-like protein as a foreign invader. Without the combination of viral infection and this genetic background, the risk of developing MS is much lower [10,11].
Together, the three papers outline a possible pathway to developing MS: EBV enters the body and infects B cells, altering their long-term behavior. In people with a particular genetic makeup, the risk of a misplaced immune response increases, resulting in T cells and EBV-infected B cells attacking myelin and disrupting its production in the brain.
These groundbreaking studies provide the first direct evidence linking EBV to multiple sclerosis. Their strength stems from relying on data from different sources: samples collected from patients, validation in an animal model to demonstrate causality, elucidation of the molecular mechanism, and the use of advanced computational tools to identify the subgroup of people who may be at increased risk.
The findings pave the way for new avenues of research aimed at combating MS: developing a vaccine against EBV, selective drugs targeting EBV-infected B cells, therapies that specifically eliminate cells marked for destroying myelin-producing cells, or early identification of at-risk individuals for treatment and monitoring. The studies reveal a plausible biological mechanism and represent an important step toward understanding MS, but achieving a safe and effective therapy will require much more research. Furthermore, the new studies demonstrate that there are complex interactions between viral infections and their long-term effects, which can give rise to entirely different diseases long after the initial infection.
Hebrew editing: Galia Halevy-Sadeh
English editing: Elee Shimshoni
References:
- Multiple sclerosis, National Institute of Neurological Disorders and Stroke
- Epidemiological cohort study on the link between Epstein-Barr virus and multiple sclerosis
- Article about the epidemiological study, Harvard School of Public Health
- B-cell overview, British Society for Immunology
- EBV-infected B cells express a protein similar to a myelin protein
- Explanatory video on the biological mechanism linking EBV to MS
- First paper—EBV-infected B cells
- T-cell overview, Cleveland Clinic
- Second paper—The dual action of T cells
- Third paper—Genetic variation
- Short video on the link between EBV and MS (new)